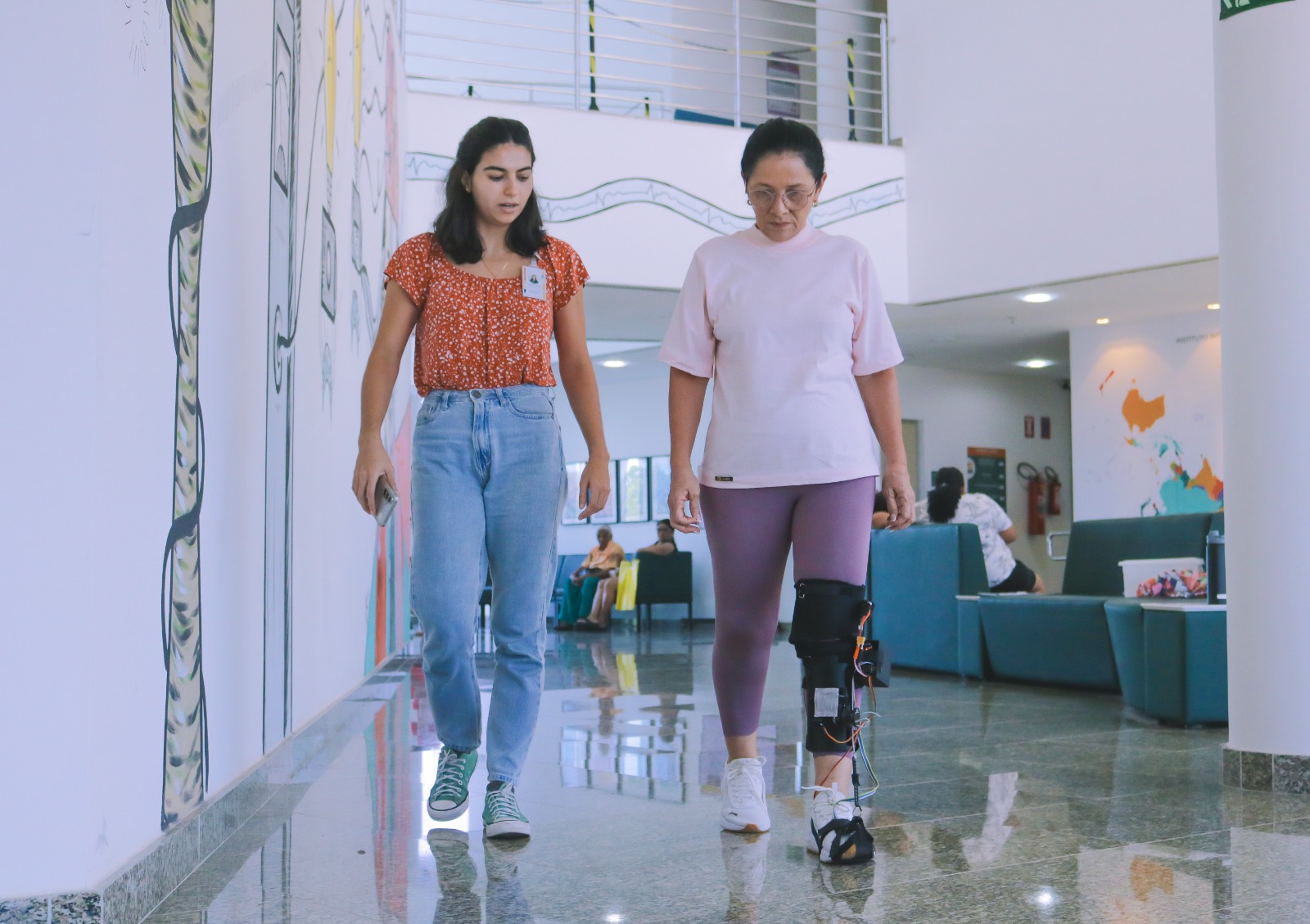Most people living with HIV/AIDS in Brazil have experienced at least one situation of discrimination throughout their lives.This is what a survey by Stigma Index towards People Living with HIV/AIDS – Brazil, where 64.1% of those interviewed confirmed that they suffered prejudice for being HIV-positive.
The data points to discrimination as one of the factors that make it difficult for people living with HIV/AIDS to adhere to appropriate treatment, says the psychologist and multidisciplinary preceptor at Anita Garibaldi Health Education and Research Center, from the Santos Dumont Institute, Carla Glenda Souza. The subject was addressed by her in her doctoral thesis in Health Sciences at the Federal University of Rio Grande do Norte (UFRN) which she defended – and was approved – this Monday (09).
The work 'Evaluation of adherence to treatment in people living with HIV/AIDS' was carried out at the Specialized Assistance Service for HIV/AIDS at Hospital Giselda Trigueiro, in Natal/RN and evaluates the factors that interfere and/or facilitate access to treatment and monitoring of people living with HIV/AIDS.
“There are difficulties in interacting with the health service, fear, and the social stigma that people with this diagnosis still carry, which is why they end up avoiding starting treatment because they deny the disease and don’t believe they are infected. This fear, this stigma that weighs heavily, even makes people change their address and create a new identity for themselves, trying to escape reality,” says the psychologist.
Graduated in Psychology from the University Center of João Pessoa and with a Master's in Health Sciences from UFRN, Carla Glenda has been working in assistance to people living with HIV/AIDS for twenty years, four of which were at Anita/ISD, where she is responsible for the Specialized Maternal and Child Assistance Service for Pregnant Women living with HIV/AIDS, Children Exposed to HIV, Children and Adolescents living with HIV/AIDS and the Service for Assistance to Victims of Sexual Violence.
According to Carla, one of the essential characteristics of the treatment for these patients is multidisciplinarity, with psychology being responsible for emotional support. “This team’s joint work is important because it provides information about the patient from the time of diagnosis onwards, which is the responsibility of the doctor, nurse, and infectious disease specialist, for example. Psychology is involved in the care and emotional support, regarding how the diagnosis was made, what the patient thinks about his/her life, and what doubts and fears exist. This way, we also identify other needs, for example, support from Social Services for some guidance, and all this support together makes the patient feel welcomed and has no fears about the treatment,” she explained.
Continuous qualification
The multidisciplinary preceptor at Anita/ISD, Carla Glenda, is part of a growing group of collaborators at the Santos Dumont Institute in a continuous process of qualification. Among the collaborators, preceptors and professors who work in the training of new professionals – students of Multiprofessional Residence or Medical Residency and internships in undergraduate courses in the health area -, 35% are masters, 26% doctors and 37% "specialists in the areas in which they work.
For the general director of ISD, Reginaldo Freitas Júnior, the example of professionals who are increasingly seeking more qualifications strengthens the Institute's performance as a school.
“ISD celebrates each of these personal victories, understanding that they are also institutional victories, as this strengthens our role as a school for health professions. The Institute is made up of people who decided to work here because they share our mission and our ideals. We always repeat the word Ubuntu as an ISD value and its meaning translates very well what we believe: I am because we are,” he said.
In December 2020, the multidisciplinary preceptor Social Worker at Anita/ISD, Alexandra Lima, also received her Master's degree in Health Education from UFRN. Alexandra developed a Matrix of common competencies for Interprofessional practice in caring for people in situations of violence, with the aim of ensuring that people in situations of sexual violence are welcomed with urgency, empathy and interprofessional care.